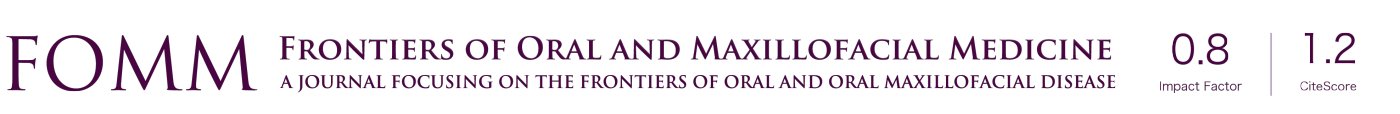Clear aligner orthognathic surgery: an overview
Introduction
Clear Aligner orthodontics has developed over the last 20 years into a viable alternative to conventional bracket and wire based orthodontia. With the advent of digital dentistry clear aligner technology has never been more prevalent. The most popular brand of clear aligners—Invisalign—documented that 5.2 million patients have worn their aligners by the end of 2017 (1). Among the many advantages for the orthodontist includes: improved financial renumeration, decreased office overhead, and increased office efficiency. Patients prefer this method of orthodontia because of the aesthetic benefit, decreased discomfort, reduced orthodontic visits, and the simplicity of changing aligners to straighten dentition (2).
As the interest in clear aligners developed, the natural progression was to attempt to use these appliances for surgical cases. Surprisingly, there are very few peer reviewed articles on clear aligner orthognathic surgery in the current literature. The earliest is from 2005, in which clear aligners were used preoperatively and postoperatively; however, just prior to surgery the patient was transitioned to conventional orthodontics for surgery (3). The author has performed clear aligner orthognathic surgery since 2016, with approximately 50 successful surgeries completed over 3 years. As such, it has become apparent that there are some significant modifications required for optimal surgical results.
These modifications can be broken down into five areas:
- Maxillomandibular fixation (MMF) intraoperatively and postoperatively.
- Post operative timing of aligner placement.
- Use of Tray splints versus conventional orthognathic splints.
- Segmental clear aligner orthognathic surgery.
- Patient specific rigid fixation/splintless surgery.
MMF intraoperatively and postoperatively is a mainstay of orthognathic surgery. It allows for stabilization of the osteotomized facial skeleton, and in conjunction with surgical splints, allows for the rigid fixation and ideal planned positioning of the maxilla and mandible. In conventional orthognathic surgery, surgical hooks attached to the orthodontic wire allows for MMF. However, clear aligner surgery is orthodontic appliance free, therefore surgical hooks are not an option.
Along the same vein, proper positioning of teeth in segmental orthognathic surgery is often guided by the surgeon’s ability to wire said dental segments into the surgical splints. Traditionally this requires the use of orthodontic fixtures and arch wires—both not available in clear aligner surgery.
Finally timing of aligner placement can be a challenge post orthognathic surgery. The orthodontic appliances used in traditional orthognathic surgery will prevent unforeseen tooth movement. With a lack of appliances, most orthodontists desire aligner placement as soon as possible post surgery to avoid unwanted tooth movement. However, in the initial weeks following surgery, mandibular range of motion is extremely limited, making placement of aligners difficult.
Determining best method for Maxillo-mandibular fixation—author’s experience
As noted above, MMF is a key component of orthognathic surgery—intraoperatively and postoperatively. Braces and associated surgical hooks are the traditional and most common method for applying MMF. Clear Aligner surgery does not provide for this scenario. Alternative methods include: Erich Arch bars, Hybrid MMF, MMF screws, and orthodontic buttons. Erich arch bars are a traditional method for completing MMF; advantages are really limited to lower cost. Disadvantages include placement time and removal time. Hybrid MMF are screw retained arch bars. Advantages include speed of placement and removal. Disadvantages include cost. Specific to orthognathic surgery, Hybrid MMF is not an ideal option due to the multiple screws needing to be placed into gingiva, which (especially in situations of segmental surgery) can compromise blood flow and blood supply to dentition and alveolar bone. MMF screws also perforate gingiva and share similar disadvantages; however not as many screws are needed as with hybrid MMF. Orthodontics buttons are attached to dentition similar to braces and act like surgical hooks; however, more often then not these buttons are not strong enough to hold 26 gauge wire. Further, buttons may be lost intraoperatively necessitating retrieval, delaying surgery (Figure 1A-1C).
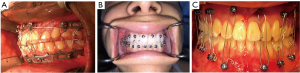
After attempting all different options, the author has found that the best option is a combination of orthodontic buttons placed on the anterior dentition and molar dentition as well as 4 MMF screws—2 superiorly, 2 inferiorly (Figure 2). Four MMF screws are quick and easy to place, and combined with a few orthodontic buttons, are enough to support MMF.
Postoperative aligner placement
Timing of aligner patient postoperatively must be discussed prior to surgery with the orthodontist, as this may impact surgical therapy. Most clear aligner orthodontists in the author’s experience desire placement of the aligner as soon as possible post surgery, provided the dental arch form has not changed during surgery. This may create an issue with patients who underwent intraoral mandibular osteotomies that are not rigidly fixated, rather heal via bony union combined with MMF, examples include inverted L osteotomies or vertical ramus osteotomies for mandibular setback. Sagittal split osteotomies or extraoral mandibular osteotomies can be rigidly fixated easily. Rigid fixation allows for a significantly quicker return to function compared to procedures requiring 4–6 weeks of MMF. As such in cases where it is desired to place postoperative aligners as soon as possible, the surgeon should consider rigidly fixating the mandibular osteotomies. It is also important to note that clear aligner placement postoperatively can cause a slight anterior open bite due to the thickness of the aligners—to minimize this open bite aligners should only be worn for 12 hours daily (Figure 3). Finally, if undergoing segmental surgery preoperative orthodontic aligners will not fit, as the arch form of the segmented jaw has changed. As such, the author has fabricated (as part of the preoperative virtual surgical planning) temporary 3D printed aligners which are placed postoperatively once the mandibular function begins to return. These temporary aligners are used until the patient can return to the orthodontist for intraoral scanning and postoperative aligner fabrication.
Tray splints and segmental surgery considerations
Traditional orthognathic surgery utilizes thin occlusal surgical splints to guide the maxilla and mandible into the presurgically determined position intraoperatively. Clear Aligner orthognathic surgery uses orthodontic retainer like tray splints which are larger and encompass more of the dental crown (Figure 4A). The author’s experience with tray splints is a positive one for non segmental surgery; segmental surgery required adjustments to the tray splint. Segmental maxillary surgery is commonly performed to correct significant skeletal malocclusion—apertognathia and transverse constriction most commonly. In traditional segmental surgery, wiring the surgical splint to the orthodontic braces and surgical hooks helps guide the osteotomized segments into the planned three dimensional position. Tray splints and a lack of orthodontic appliances do not permit this technique for positioning the dental segment. As such, placement of osteotomized segments into the tray splints can be challenging, but not impossible. This often requires significant manipulation of both the splint and dental segment. Tray splints, however, are not as rigid as traditional orthognathic splints. Flexion of the splint may occur during larger segmental movements, placing the maxillary segment in an incorrect position. For example, in a case with an 8-mm transverse expansion planned, the tray splint was not rigid, resulting in flexion, ultimately placing the maxillary segments in a position in which the 8 mm expansion was not obtained and the right sided posterior cross bite was not corrected. Expansion had to be performed without the splint—not ideal, requiring multiple attempts at rigid fixation, adding significant time to the surgery (Figure 4B). As such the author advocates for segmental clear aligner orthognathic surgery adding a palatal strap to the tray splint, to decrease flexion and increase rigidity (Figure 4C). The palatal strap is rigid enough to minimize unwanted three dimensional movements of the maxilla postoperatively.
Patient specific rigid fixation
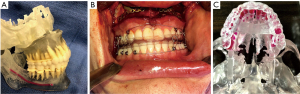
Technology has made the planning of maxillofacial surgery entirely digital. Virtual surgical planning has become a standard of care for the maxillofacial surgeon—turning several hours of dental lab work into as little as a 15-minute remote planning session (4). Further, digital technology has evolved to the point that patient specific, 3D printed rigid fixation is also becoming the standard of care (5). Clear aligner orthognathic surgery fits naturally with both of these technological advancements—cone beam based maxillofacial CT scans and intraoral digital scans of dentition are both required in clear aligner orthodontics and virtual surgical planning. Patient specific rigid fixation is truly a “game changer” for maxillary orthognathic surgery, especially clear aligner orthognathic surgery. This technology allows for splintless surgery—making orthognathic procedures more efficient and avoiding some of the splint related issues noted above. The author’s standard protocol is as follows: through a remote planning session, a custom marking guide and associated patient specific rigid fixation plate is designed. The marking guide is placed on the exposed maxilla intraoperatively. On the marking guide are slots to place the LeFort osteotomy, as well as cylinders to mark planned screw placement. This ensures that the Lefort osteotomy and associated fixation holes are aligned to allow the patient specific rigid fixation plate to place the down fractured and mobile maxilla into the proper position without the use of a surgical splint (Figure 5A-5C). Of note when using patient specific implants for segmental LeFort osteotomies, the plate only provides stability in one vector, therefore complete stabilization with a tray splint of conventional splint may be necessary.

Conclusions
Clear aligner orthodontia is becoming a modality of choice among orthodontists globally. While once limited to non-surgical orthodontics, in the last 3–4 years, more and more orthodontists are advocating clear aligner surgery to their patients, and in turn, the maxillofacial surgeon. As such, it behooves the surgeon to adapt and adjust to non-orthodontic appliance based orthognathic surgery. While there are some significant adjustments to be made, technological advancements (in particular patient specific rigid fixation) have made clear aligner surgery the future of orthognathic surgery.
Acknowledgments
Funding: None.
Footnote
Provenance and Peer Review: This article was commissioned by the Guest Editor (Sung-Kiang Chuang) for the series “Clinical Outcomes and Innovations in Oral and Maxillofacial Surgery” published in Frontiers of Oral and Maxillofacial Medicine. The article has undergone external peer review.
Peer Review File: Available at https://fomm.amegroups.com/article/view/10.21037/fomm-21-18/prf
Conflicts of Interest: The author has completed the ICMJE uniform disclosure form (available at https://fomm.amegroups.com/article/view/10.21037/fomm-21-18/coif). The series “Clinical Outcomes and Innovations in Oral and Maxillofacial Surgery” was commissioned by the editorial office without any funding or sponsorship. SRA is the President of NJ Society of OMS. The author has no other conflicts of interest to declare.
Ethical Statement: The author is accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Align Technology Corporate Fact Sheet 2017. Accessed April 27, 2020. Available online: https://www.aligntech.com/documents/Align%20Technology%20Corp%20Fact%20Sheet%202017%20Q4F.pdf
- Weir T. Clear aligners in orthodontic treatment. Aust Dent J 2017;62:58-62. [Crossref] [PubMed]
- Boyd RL. Surgical-orthodontic treatment of two skeletal Class III patients with Invisalign and fixed appliances. J Clin Orthod 2005;39:245-58. [PubMed]
- Farrell BB, Franco PB, Tucker MR. Virtual surgical planning in orthognathic surgery. Oral Maxillofac Surg Clin North Am 2014;26:459-73. [Crossref] [PubMed]
- Suojanen J, Leikola J, Stoor P. The use of patient-specific implants in orthognathic surgery: A series of 32 maxillary osteotomy patients. J Craniomaxillofac Surg 2016;44:1913-6. [Crossref] [PubMed]
Cite this article as: Aziz SR. Clear aligner orthognathic surgery: an overview. Front Oral Maxillofac Med 2022;4:24.